Blog Post
The True Cost of Cancer
Color

Cancer Costs Us Everything
Cancer is a terrifying word and a heartbreaking experience. Nearly everyone has been affected by it — too many people have lost loved ones or have faced the arduous journey of survival themselves. The latest statistics are grim — one in two women, and one in three men, will be diagnosed with cancer at some point in their lives. For every cancer diagnosis, countless family members, friends, and colleagues walk beside the patient. Cancer hurts all of us.
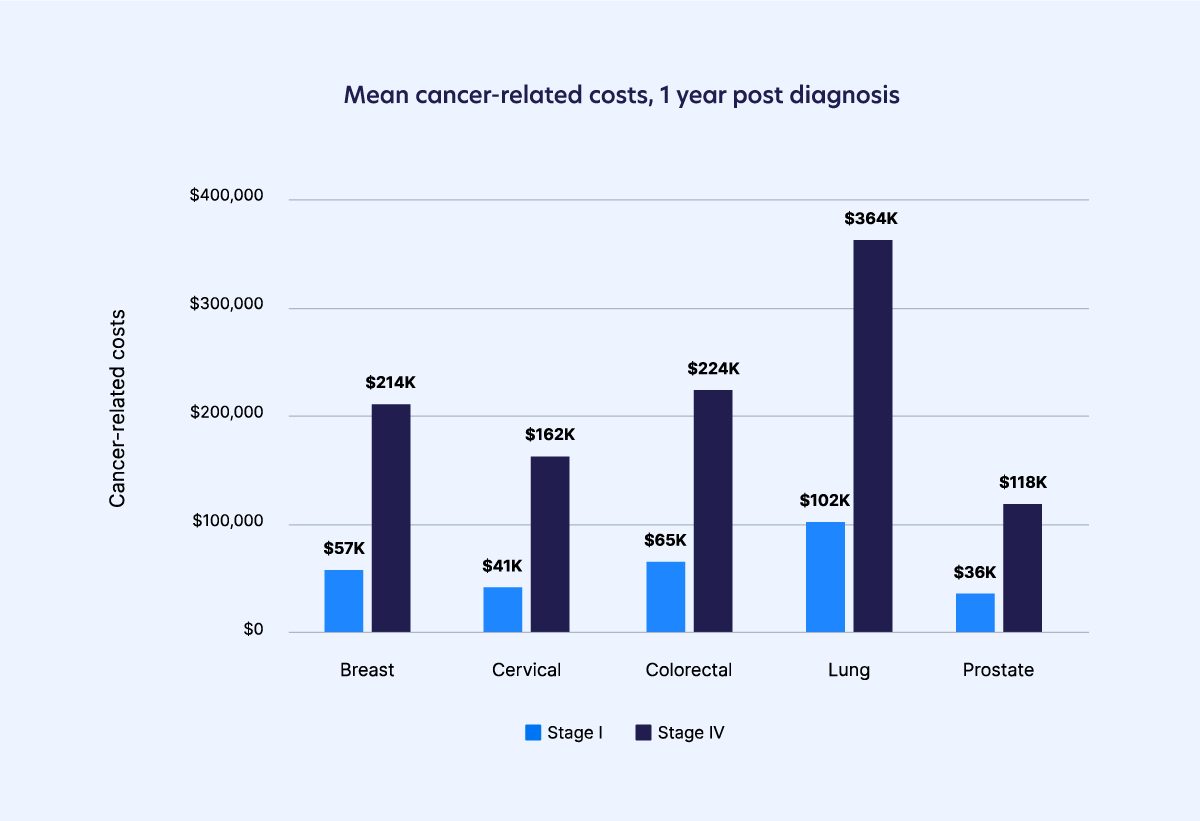
The financial burden compounds the physical and emotional toll of cancer. Even for patients with health insurance, the out-of-pocket costs are staggering. Breast cancer treatment, for example, costs insured patients an average of roughly $140,000 — an increase of 29% over the last five years. These ballooning costs strain the entire economy through increased total health care costs for employers. The average costs that U.S. employers pay for their employees’ health care will increase 6.5 percent to more than $13,800 per employee in 2023.
Cancer has become the most costly contributor to employee health care costs. The cost of cancer treatments, including medications and medical procedures, is higher than other health care costs. Employee health care costs for those diagnosed with cancer are four to five times higher than costs for other employees, and estimates put the total employer spending for cancer treatment at 180 billion dollars. As a result, employers need to make arrangements to cover these costs or risk leaving their employees without the necessary treatments they require.
Many Cancer Deaths are Preventable
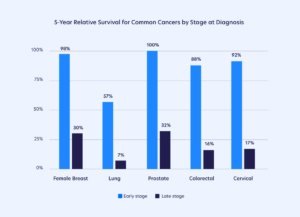
Preventing cancer is always better than getting to the point of needing treatment. This is not an impossible goal, given that the World Health Organization estimates that between 30%-50% of all cancers worldwide are due to elements within our control. Further, the likelihood of successful cancer treatment for the most common cancers is quite high. The latest research from the American Cancer Society estimates that the 5-year survival rate for the most common form of breast cancer is 99% when detected early. Early detection also leads to a 92% and 98% 5-year survival rate for cervical and prostate cancers, respectively. Among all these cancers, the survival rate plummets to 50% or lower when the cancers progress to later stages.
Preventive screenings are underutilized, and the trends are moving in the wrong direction. Back in 2015, an investigation found that only 8.5% of adults over 35 received all recommended, high-priority preventive care screenings. By 2018, 6.2% of adults received appropriate care. In 2020, only 28 states met the CDC’s Healthy People goals for Colorectal Cancer Screenings. Nine in ten Americans that same year were behind on their lung cancer screenings. The COVID-19 pandemic accelerated this downward trajectory. A recent paper published by the National Institutes of Health found devastating declines in all cancer screenings in the United States and worldwide. In the US, screenings for breast, colon, prostate, and lung cancer screenings were lower by 85%, 75%, 74%, and 56%, respectively. Researchers estimate that the COVID-19 pandemic is responsible for 25% higher cancer mortality and that most of these excess deaths will occur before 2025.
Our Commitment to a Cancer-Free Future
At Color, we are putting every resource we have into creating a cancer-free future. The mission is clear — get more people up to date on recommended screening guidelines and close the gaps between screening, diagnosis, and timely treatment. Color’s approach to cancer prevention and screening focuses on three fundamental goals:
Get more people to the proper screenings and make those screenings convenient.
In a survey of 2,000 unscreened adults, the American Cancer Society found clear patterns when investigating why some people avoid cancer screenings. The authors focused on colorectal cancer, one of the cancers most survivable with early detection. While awareness about the guidelines for screening was very high (nearly 100%), researchers found that knowing we should do something doesn’t always mean we will. Those surveyed expressed fear of the test itself, as well as embarrassment about the procedure. Many respondents believed the screening was only recommended if they had symptoms or a family history of the disease. Many folks also felt the screening “wasn’t worth it” due to the complexity of arranging time off work, getting child care, transportation, and other logistics. We cannot end cancer without confronting these very human fears and challenges.
Ensure that nobody gets lost along the way and shorten the critical period between screening and follow-up care.
The cancer journey can feel isolating, even if a patient walks through it with friends and family. The word “cancer” can make us feel helpless. That’s why every person facing cancer deserves an advocate. Care navigation is a crucial component of any whole-person cancer solution. Three decades of robust studies support the importance of patient navigators — trained, empathetic lay workers who help patients traverse the cancer care continuum. The very first of these studies measured the life-saving effect of patient navigators assisting black women in poverty in Harlem. At the time, black women were dying at extraordinarily high rates of the disease, often presenting for their first appointment at advanced disease stages. Assigning patient navigators to get more women screened early and often and stay alongside them through diagnosis and treatment nearly doubled the five-year survival rate. Patient navigators, or care advocates, are irreplaceable team members in the fight for health equity.
At Color, we believe we are called to use the infrastructure we’ve developed over the last decade to bring the best cancer prevention and screening tools to more people in more places.
If you want to join this challenge and learn more about our vision for a cancer-free future, reach out at learnmore@color.com.