Blog Post
Every health benefits plan should include a tiered cancer prevention program. Here’s how one looks.
Color

In the U.S., cancer is the number one healthcare cost for employers and unions. The vast majority of this burden comes from treating late-stage cancers.
Not every employee will experience late-stage cancer. Hopefully very few do. But to truly tackle cost, employers need to deploy a comprehensive, tiered strategy that narrows their efforts—screening everyone eligible, and then providing the most targeted resources for those at greatest risk for developing late-stage cancer.
Here’s what that might look like:
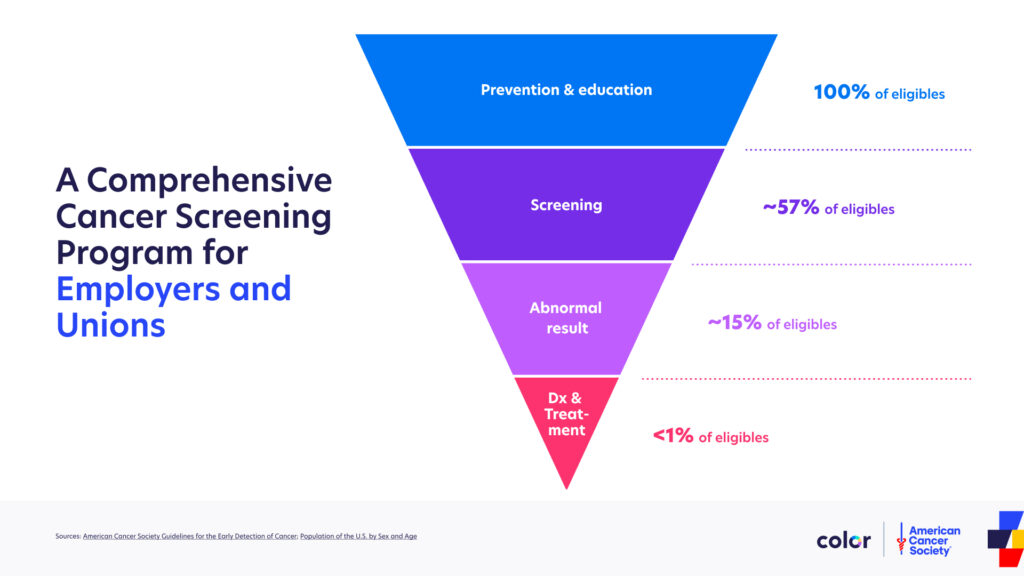
In this example, the entire company (100%) starts by receiving personalized risk assessments, educational resources, and support for well-known prevention methods (think: smoking cessation programming).
After that, those eligible for recommended screenings based on age and family history (say, 57% of workers) are led through easy-to-manage screenings for major cancers—breast, cervical, lung, prostate, and colorectal. This is a mix of at-home screenings and booking of in-person screenings—with much faster times to get in the door than traditionally happens. For higher-risk employees, it can also include genetic testing. The genetic tests—which are covered by insurance—can help ensure that high-risk individuals get screened for cancer earlier than they would have otherwise.
From there, all resources are focused on addressing abnormal results (in, say, 15% of workers). For this sliver of the workforce, the program provides on-demand consultations with physicians, clinical orders for follow-up testing, and Dedicated Care Advocates.
By homing in on the factions of a workforce that are at greatest risk for cancer, employers can get ahead of the looming financial burden of late-stage cancer. Many employers know this is already the state of affairs. In fact, about 44% of employers expect to see a rise in late-stage cancer in their ranks. It’s a trend that should not be met with a shoulder shrug. It’s one that should be nipped in the bud at all costs.



